Recurrent Miscarriage Causes: Why It Happens and What Helps
She walks into the clinic carrying more than a medical history. After a second loss, sometimes a third, the question on her mind is rarely about test reports. It is quieter, harder, and almost always the same: why does this keep happening to me.
In clinical practice, that question is where every meaningful conversation about repeated pregnancy loss begins. The grief in the room is real, but so is the gap between what a woman feels and what a structured medical evaluation will reveal. One does not cancel the other.
 Many women arrive believing the losses are their fault, or that nothing more can be done. Both assumptions are wrong. Recurrent miscarriage is a recognised medical category with an established evaluation pathway, and in a meaningful share of cases, an identifiable and treatable cause.
Many women arrive believing the losses are their fault, or that nothing more can be done. Both assumptions are wrong. Recurrent miscarriage is a recognised medical category with an established evaluation pathway, and in a meaningful share of cases, an identifiable and treatable cause.
This article explains the most common recurrent miscarriage causes, how evaluation and testing actually work, and what treatment looks like — so the next step becomes a clinical decision, not a guess.
Also Read:
- Missed Abortion Explained: Causes, Symptoms, and Recovery
- Biochemical Pregnancy: Positive Test Without Pregnancy
- Bleeding in Early Pregnancy: Symptoms, Causes, and Outcomes
Understanding Recurrent Miscarriage
Recurrent miscarriage is medically defined and clinically specific. It is not a term used for every difficult pregnancy experience. Understanding the definition is the first step in approaching evaluation and care with clarity, calm, and a clear direction.
Recurrent miscarriage refers to two or more consecutive pregnancy losses before 20 weeks requiring structured medical evaluation.
What Recurrent Miscarriage Means Medically
Recurrent miscarriage refers to two or more consecutive pregnancy losses before 20 weeks of gestation. Earlier definitions required three losses, but current international and Indian obstetric consensus supports evaluation after two. Earlier evaluation allows underlying factors to be identified sooner and improves the planning of the next pregnancy.
This is distinct from a single, sporadic miscarriage. A first-trimester loss is common, often caused by random chromosomal errors, and does not by itself indicate a medical pattern. Recurrent loss, by contrast, is a pattern that deserves structured medical attention.
Why It Deserves Structured Evaluation
Repeated pregnancy loss is often described in everyday language as bad luck. In clinical practice, it is more accurately a question. A specific cause can be identified through evaluation. In others, no single cause is found, and that itself is a meaningful clinical finding.
Either outcome guides care. Identifying a cause directs treatment; not finding one supports a different kind of care, focused on monitoring and reassurance in the next pregnancy. Both are clearer paths than the uncertainty most women begin with.
Recurrent miscarriage is a recognised clinical category with a structured medical response. Defining it correctly opens the door to evaluation, identifiable causes, and a path forward that does not rely on chance, self-blame, or fragmented advice from unreliable sources.
 Common Recurrent Miscarriage Causes
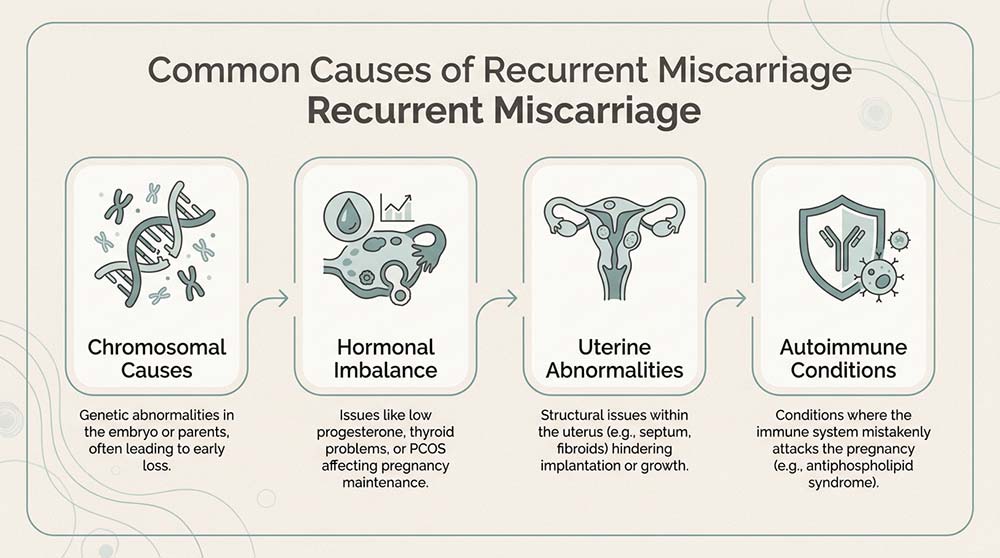
Common Recurrent Miscarriage Causes
Most recurrent miscarriage causes are linked to a few clearly recognised medical categories. Each carries different implications for evaluation and treatment, and many can be identified through standard investigations performed under specialist supervision.
Chromosomal and Genetic Factors
Chromosomal factors remain the single largest contributor to early pregnancy loss, including in women experiencing repeated miscarriage. Some are random events. Others are inherited and identifiable through testing.
- Random chromosomal errors: The single most common cause across all miscarriages, including a meaningful share of recurrent losses.
- Parental chromosomal translocations: Less common but identifiable through karyotyping; explains repeated losses in a defined group of couples.
- Maternal age: Chromosomal risk rises with age — a clinical reality acknowledged plainly, not framed as alarm.
Uterine, Hormonal, and Immunological Factors
Beyond genetics, several well-studied medical categories account for recurrent loss. Each is identifiable through specific investigations and, where present, has an established management approach.
- Uterine anatomical factors: Septate uterus, fibroids in specific locations, or intrauterine adhesions can affect implantation and early pregnancy progression.
- Hormonal and endocrine factors: Thyroid disorders, uncontrolled diabetes, and PCOS-related metabolic issues can disrupt early pregnancy support.
- Immunological factors: Antiphospholipid syndrome is the most clinically significant immune-related cause and is identifiable through blood testing.
- Lifestyle and environmental factors: Often discussed in general health terms, but rarely the sole cause of recurrent pregnancy loss.
Recurrent miscarriage causes span genetic, anatomical, hormonal, and immunological categories. Understanding which category applies in an individual case is what evaluation is designed to determine — clearly, methodically, and without guesswork or assumptions.
Evaluation and Investigations
A structured recurrent pregnancy loss evaluation and carefully selected tests for recurrent miscarriage help doctors move from possibility to clarity.The tests are well-established, follow a logical sequence, and are designed to answer specific clinical questions in a defined order.
The Standard Tests for Recurrent Miscarriage
The tests for recurrent miscarriage are organised around the major cause categories. Parental karyotyping addresses genetic factors. Pelvic imaging — beginning with ultrasound, and where indicated extending to hysteroscopy or saline sonography — evaluates uterine anatomy. Hormonal and thyroid panels assess endocrine function. Blood tests for antiphospholipid antibodies cover the most clinically significant immunological cause. These investigations are not run all at once. They are chosen, sequenced, and interpreted in clinical context, with each result shaping what is examined next. The goal is a focused answer, not an exhaustive panel.
When should evaluation for recurrent miscarriage begin?
Evaluation is generally recommended after two consecutive pregnancy losses. Earlier referral may be appropriate where maternal age or specific clinical concerns are present. The goal is to identify a treatable cause where one exists, and to provide medically grounded reassurance where one does not.
Evaluation is not a single test but a sequence — chosen carefully, interpreted in clinical context. Results may identify a cause, narrow the possibilities, or confirm that no specific abnormality is present, each of which directs the next step in care.
Treatment and Future Pregnancy Planning
Recurrent miscarriage treatment is guided by what evaluation reveals. Most identified causes have established management approaches, and women with no identified cause still carry a strong likelihood of a successful future pregnancy under structured doctor-led care.
Treatment Aligned to the Identified Cause
Treatment is most effective when matched precisely to the cause. Chromosomal translocations are managed through genetic counselling and reproductive options chosen with specialist guidance. Uterine anatomical issues may be addressed through surgical correction where clinically indicated. Hormonal and endocrine factors are optimised before the next conception.
Antiphospholipid syndrome has established medical management delivered under specialist care. Where no specific cause is identified — a recognised clinical category in itself — care focuses on close early monitoring and supportive measures, with an overall outlook that remains generally favourable.
Planning the Next Pregnancy with Confidence
Pre-conception planning matters. Addressing identified factors, optimising general health, confirming pregnancy early, and establishing structured early monitoring all contribute to a clearer next pregnancy. None of this is about doing more for the sake of it. It is about doing the right things at the right time.
Anxiety in a subsequent pregnancy is normal and clinically anticipated. Care plans typically account for it through earlier scans, closer follow-up, and unhurried consultations. The emotional dimension is not separate from medical care — it is part of how good care is delivered.
Treatment is most effective when matched precisely to the identified cause, and even unexplained recurrent loss carries a generally favourable outlook with proper guidance. Planning the next pregnancy with medical supervision replaces uncertainty with a clearly defined path.
Also Read:
- Blighted Ovum Causes Symptoms and Diagnosis Explained
- What to Expect in Pregnancy After Recurrent Miscarriage
Conclusion
Recurrent miscarriage causes are identifiable in many cases, and the medical pathway is more structured than most women realise when they first walk into a clinic. A defined evaluation, targeted tests for recurrent miscarriage, and treatment matched to the underlying cause together transform a difficult history into a clear clinical plan. Where no specific cause is found, structured care and close monitoring continue to support healthy future pregnancies.
If you have experienced two or more pregnancy losses, a structured evaluation can give you the clarity and guidance your next step deserves. Book a consultation today for personalised, doctor-led care.
Our Digital Imprints:
Dr. Madhu Goel
Senior Consultant Obstetrician and Gynaecologist
Director, Fortis La Femme
I am passionate about women’s health and believe that informed, compassionate care empowers women to make confident choices. With experience in high-risk pregnancies, infertility, and gynaecological care, my focus remains on guiding patients with clarity, empathy, and trust.
Stay informed with Health Hub, my newsletter dedicated to women’s health and wellness, where I share evidence-based insights and practical guidance.
You can also connect with me on Instagram | Facebook | LinkedInfor regular updates on women’s health.





