Biochemical Pregnancy: Positive Test Without Pregnancy
A positive pregnancy test followed by an empty ultrasound can feel confusing and disheartening. You prepared for a pregnancy. The tests confirmed it. Yet the scan showed no gestational sac, no embryo, no visible pregnancy at all. This is often described as a positive pregnancy test but no pregnancy on scan.
In my clinical practice as an obstetrician and gynaecologist, this is one of the most misunderstood situations women face in early pregnancy. The medical explanation is clear, but the emotional confusion often comes from the gap between what the body signals and what the scan shows.
 This situation is medically known as a biochemical pregnancy, also called chemical pregnancy. It is among the most common forms of early pregnancy loss, yet one of the least discussed, because it often resolves before a woman even realises she is pregnant.
This situation is medically known as a biochemical pregnancy, also called chemical pregnancy. It is among the most common forms of early pregnancy loss, yet one of the least discussed, because it often resolves before a woman even realises she is pregnant.
In this article, I explain what biochemical pregnancy means, the common biochemical pregnancy causes, how the condition is diagnosed, what biochemical pregnancy symptoms look like, and how women can approach recovery and the next pregnancy with confidence.
Also Read:
- Blighted Ovum Causes Symptoms and Diagnosis Explained
- Miscarriage Causes, Symptoms, Recovery, and Future Pregnancy Planning
What Biochemical Pregnancy Means
Biochemical pregnancy is a very early pregnancy loss where beta hCG levels rise enough to give a positive test, but the pregnancy stops developing before it becomes visible on ultrasound. It usually occurs before five weeks and resolves naturally.
Biochemical pregnancy is confirmed by hormonal testing rather than imaging. The pregnancy stops progressing so early that beta-hCG can be detected in the blood and urine before the gestational sac becomes visible on ultrasound.
A positive pregnancy test with no pregnancy on ultrasound is often searched by women. In medical terms, this is known as a biochemical pregnancy.
Why Pregnancy Tests Turn Positive Despite No Visible Pregnancy
In a normal cycle, the egg is released from the ovary, fertilised in the fallopian tube, and the resulting pregnancy travels down into the uterus where it implants. Once implantation begins, the early placental cells start releasing beta-hCG, the hormone that turns the urine and blood pregnancy tests positive.
In a biochemical pregnancy, this same sequence begins. The pregnancy implants, beta-hCG rises, and every test says pregnant. But the pregnancy stops growing before it is large enough to be seen on ultrasound. The hormone is real. The implantation was real. The progression simply did not continue.
 How Common Biochemical Pregnancy Really Is
How Common Biochemical Pregnancy Really Is
Biochemical pregnancy is far more common than most women realise. It is estimated that nearly 25 percent of all pregnancies end in loss before 20 weeks, and a significant share of these are biochemical pregnancies occurring in the first few weeks.
The exact number is difficult to measure. Many women never know they were pregnant. A period may arrive two, four, or five days late. It may feel absolutely normal, or slightly heavier than usual, and that is the end of it. Without a pregnancy test in that window, the biochemical pregnancy goes entirely unrecognised.
Understanding biochemical pregnancy begins with recognising that pregnancy can be chemically active before it becomes visible on ultrasound. This distinction helps women interpret early test results with clarity rather than assuming something has been missed or done wrong.
Why Biochemical Pregnancy Happens (Causes)
Most biochemical pregnancy causes are rooted in early developmental biology. The fertilised egg cannot progress beyond the earliest stages of pregnancy, and in most cases this is a natural biological response rather than a reflection of anything the woman did or did not do.
Chromosomal Abnormalities as the Main Cause
The most common cause of biochemical pregnancy is a chromosomal abnormality. This means either there was a problem with the egg, a problem with the sperm, or an error during fertilisation. The resulting embryo does not carry the genetic structure required to develop further, and the body recognises this very early.
These chromosomal events are random. They are not caused by stress, daily activity, food, travel, or anything the woman did in the days around conception. The pregnancy does not progress because it was never biologically viable from the earliest stage.
Other Possible Factors
A smaller share of biochemical pregnancies may be linked to other factors. An abnormal uterus or inadequate uterine lining may not support implantation well enough for the pregnancy to continue. Hormonal disorders, where the body’s hormone levels are fluctuating outside normal ranges, can also contribute in some cases.
These secondary factors are usually identified through routine gynaecological evaluation, and in most cases, they can be addressed before planning the next pregnancy.
Understanding biochemical pregnancy causes helps shift the conversation from self-blame to medical clarity. These are biological events the body manages on its own, and for the vast majority of women, they do not indicate any lasting reproductive concern.
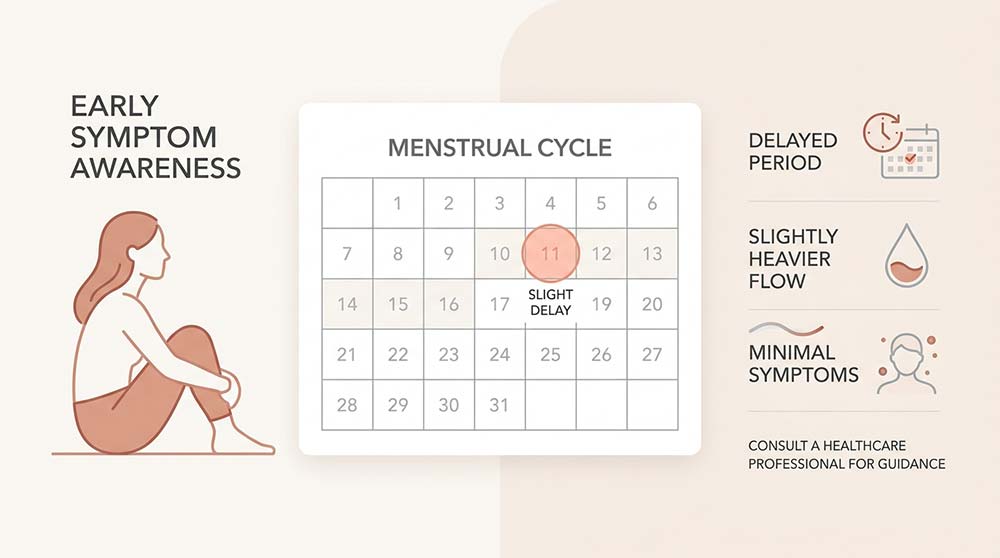 Recognising Biochemical Pregnancy Symptoms
Recognising Biochemical Pregnancy Symptoms
Biochemical pregnancy symptoms are often minimal or absent. For most women, the loss presents as a period that arrives slightly late or with slightly heavier bleeding than usual, without any clear sign that a pregnancy had even begun.
Why Symptoms Often Go Unnoticed
Biochemical pregnancy typically occurs before five weeks of gestation. At this stage, most women have not yet experienced any noticeable pregnancy signs such as nausea, fatigue, or breast tenderness. The period may simply arrive a few days late, or it may appear on time but feel heavier than a usual cycle.
This is why so many biochemical pregnancies are never identified. Without a sensitive pregnancy test taken early, there is no clinical signal to capture the brief window during which the pregnancy was active.
When Women Are Most Likely to Recognise It
Biochemical pregnancy is most often identified in women who are actively trying to conceive, women undergoing IVF, and women who take pregnancy tests very early in the cycle, sometimes even before a missed period. In these cases, the initial test is positive, but the follow-up beta-hCG blood test shows that hormone levels are not rising as expected.
Because symptoms are rarely distinct, biochemical pregnancy is underdiagnosed in the general population. For women closely monitoring conception, recognising the signs early allows for appropriate clinical follow-up and calm medical reassurance.
Can a Positive Pregnancy Test Show No Pregnancy?
Yes, a positive pregnancy test can show no pregnancy in cases of biochemical pregnancy. In this situation, beta hCG levels rise enough to make urine and blood tests positive, but the pregnancy stops developing very early. Because this happens before five weeks, nothing is seen on ultrasound. This often leads to confusion, as tests suggest pregnancy while the scan appears normal. Medically, this is considered an early pregnancy loss. It is important to understand that this is a natural biological process and not caused by anything the woman did. Proper follow up with your doctor helps confirm the diagnosis and provides reassurance.
How Biochemical Pregnancy Is Diagnosed
Diagnosis of biochemical pregnancy relies on hormonal trends rather than imaging. Because the pregnancy resolves before it becomes visible on ultrasound, serial beta-hCG testing is the primary tool, with ultrasound used to support the overall clinical picture.
Role of Serial Beta-hCG Testing
In a normally progressing pregnancy, serum beta-hCG should rise by at least 66 percent over 48 hours. This rising pattern reflects a healthy early pregnancy. In a biochemical pregnancy, the beta-hCG does not rise as expected. Instead, levels plateau, or they begin to fall. This falling or stalling pattern is what confirms the diagnosis.
This is why two blood tests are often better than one when an early pregnancy result is in question. A single positive test confirms that implantation occurred. The trend over 48 hours shows whether the pregnancy is progressing.
Why Ultrasound Shows Nothing in Biochemical Pregnancy
Because biochemical pregnancy resolves before five weeks of gestation, the ultrasound does not show a gestational sac, an embryo, or cardiac activity. The uterus appears empty on the scan, even though the blood tests are positive. This mismatch is one of the most emotionally difficult parts of the diagnosis for many women.
In clinical practice, the combination of rising-then-falling beta-hCG and an empty ultrasound is a clear picture. It is not a missed pregnancy, and it is not a scan performed too early without reason. It is a pregnancy that ended before imaging could visualise it.
Accurate diagnosis of early pregnancy loss depends on combining hormonal data with imaging and clinical judgment. This evidence-based approach protects women from misdiagnosis and supports calm, informed decisions about what comes next.
Recovery and Planning the Next Pregnancy
Recovery after a biochemical pregnancy is usually straightforward. The body resolves the pregnancy on its own, and with appropriate medical follow-up, most women go on to have healthy pregnancies without any lasting impact on fertility.
Why the Body Resolves It Without Intervention
In almost all cases of biochemical pregnancy, no medical treatment is required. The body lets go of the pregnancy naturally. A heavy period comes, or sometimes a normal period, and that marks the end of the biochemical pregnancy. There is no medication to take, no procedure to undergo, and no complication to manage for the vast majority of women.
Preparing for the Next Pregnancy Under Medical Guidance
Biochemical pregnancy should be treated as an early abortion in terms of recovery planning. Women are generally advised to wait at least one to two menstrual cycles before trying to conceive again. This allows the body to return to its natural cycle rhythm and supports a healthier start to the next pregnancy.
Before planning the next pregnancy, a visit to the gynaecologist for a routine check-up is important. This ensures there are no underlying conditions that need attention, such as hormonal imbalance or uterine concerns. Folic acid supplementation should be started before conception, and with that preparation in place, the next pregnancy can be approached with confidence.
Biochemical pregnancy does not affect future fertility for most women. With calm medical guidance and structured preparation, the next pregnancy can be approached with clarity, informed expectations, and appropriate clinical support throughout.
 Conclusion
Conclusion
Biochemical pregnancy is an early form of pregnancy loss confirmed by hormonal testing rather than ultrasound imaging. It most often occurs due to chromosomal abnormalities in the fertilised egg and reflects a natural biological response rather than a health failure.
Biochemical pregnancy symptoms are often minimal and may present only as a slightly late or heavier period, making this early pregnancy loss easy to miss. Diagnosis depends on serial beta hCG levels and ultrasound findings showing no pregnancy. Recovery is usually natural, with the body resolving the biochemical pregnancy on its own.
Under doctor-guided follow-up, future pregnancies are generally unaffected, and most women go on to have healthy outcomes.
Book a consultation with Dr. Madhu Goel for clear, expert-led guidance on early pregnancy loss and planning your next pregnancy with confidence.
Our Digital Imprints:
Dr. Madhu Goel
Senior Consultant Obstetrician and Gynaecologist
Director, Fortis La Femme
I am passionate about women’s health and believe that informed, compassionate care empowers women to make confident choices. With experience in high-risk pregnancies, infertility, and gynaecological care, my focus remains on guiding patients with clarity, empathy, and trust.
Stay informed with Health Hub, my newsletter dedicated to women’s health and wellness, where I share evidence-based insights and practical guidance.
You can also connect with me on Instagram | Facebook | LinkedInfor regular updates on women’s health.